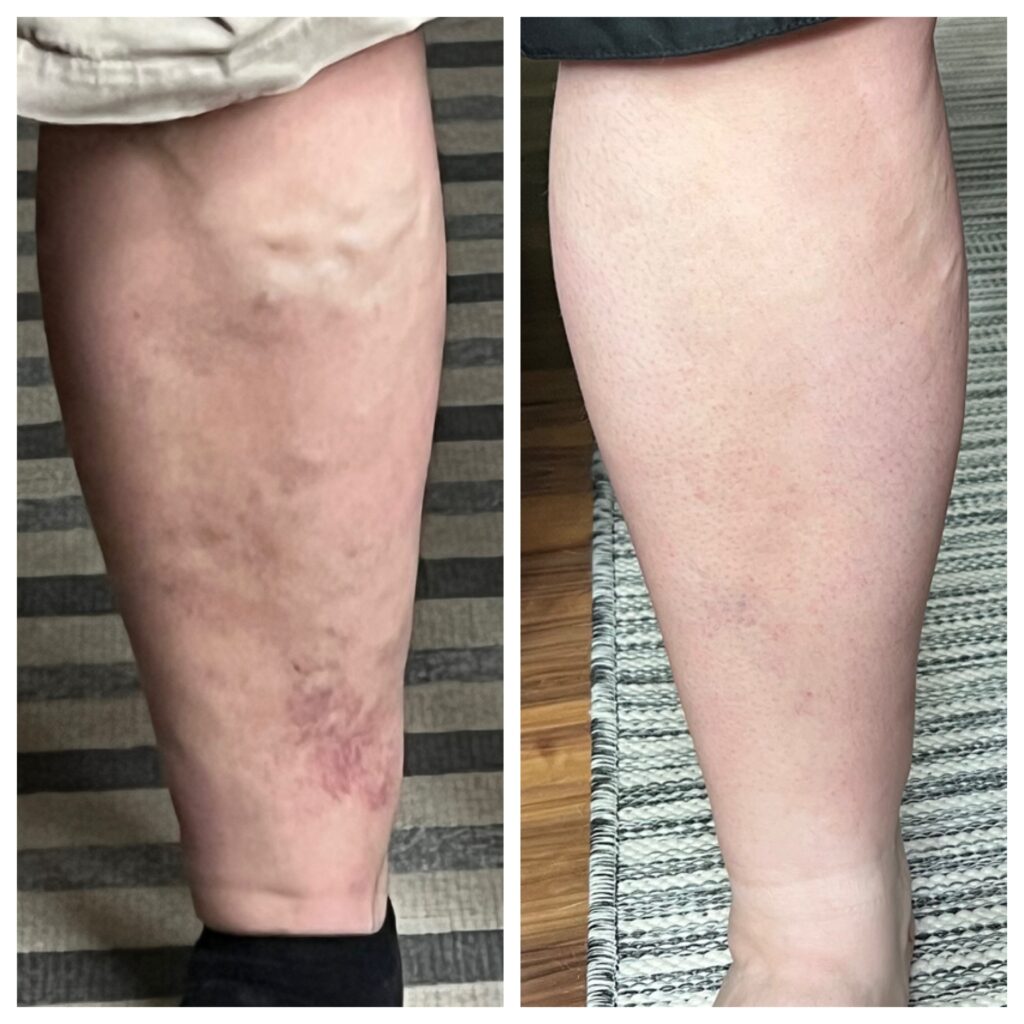
An estimated 40 percent of people in the United States have chronic venous insufficiency. Venous insufficiency can present itself as a spider or varicose veins and may be a sign of significant underlying venous disease.
Venous insufficiency can be the result of heredity, age, gender, weight, history of deep vein thrombosis (blood clots), multiple pregnancies, inactivity and occupations that require prolonged sitting or standing.
At the Metropolitan Vascular Institute, our knowledgeable providers offer varicose vein treatment for your venous insufficiency. Call (301) 374-8540 today to learn more or to determine whether you are a candidate for treatment!
*Rights reserved with the owner of the video
What are varicose veins?
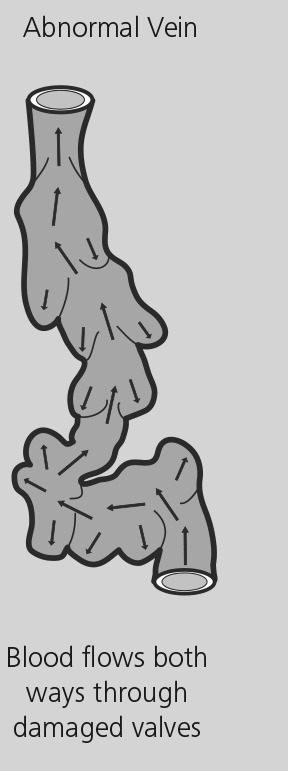
When the veins are damaged, gravity will hinder normal blood flow causing blood to form pools in the weakened, damaged veins. The pooling blood causes these veins to enlarge. Twisted masses of veins beneath the surface of the skin, known as varicose veins, often result.
Varicose veins are larger and located deeper in the leg than spider veins. Spider veins are small red, blue and purple veins on the surface near the skin.
What are the Symptoms of Varicose Veins?
- Aching/Pain
- Heaviness
- Tiredness/fatigue
- Itching/Burning
- Swollen ankles
- Leg cramps
- Restless legs
- Throbbing
Who is the ideal candidate for Varicose Vein Treatment?
Anyone who wants to get rid of uncomfortable varicose veins may be a good candidate for one of the available forms of treatment. Vein treatments are not performed on women who are pregnant. In many pregnancy-related cases, the condition resolves over the course of 3 to 4 months.
Certain medical conditions may prevent the safe administration of varicose vein treatment, as well, such as significant cardiovascular disease.
Our vein specialists conduct a thorough consultation, health history, and examination to ensure that treatment can be safely performed on each of our patients.
Frequently Asked Questions
How are varicose veins treated?
There are generally 2 treatment options:
- Conservative measures such as the use of compression stockings and change in lifestyle
- Corrective treatment such as endovenous laser therapy, ambulatory phlebectomy, and sclerotherapy.
What Happens If Varicose Veins Are Left Untreated?
Once they have developed, varicose veins will usually worsen with time. This is true even if you make lifestyle changes to control them and to manage the pain. In most cases, these veins are simply unsightly, but they don’t cause long-term medical problems.
In some cases, however, varicose veins can lead to ulcers or sores on your legs, blood clots, or chronic inflammation. If any of these symptoms develop, your varicose veins need to be treated and removed. When your varicose veins are a part of chronic venous insufficiency, not paying attention and treating them can be very risky for your health.
Who Is at Risk for Developing Varicose Veins?
The passage of time and pregnancy are the two main causes of varicose veins.
- Aging — As we age, our vein walls lose some of their elasticity. This not only allows them to stretch, but it also means they won’t move the blood as effectively. Our muscles that help push the blood weaken, as well.
- Pregnancy — Some women develop varicose veins in pregnancy. This is because pregnancy increases the volume of blood in the body but decreases the flow of blood from the legs to the pelvis. While this is good for the developing fetus, it’s bad for the appearance of the legs when varicose veins form. Varicose veins in pregnant women usually improve on their own from 3-12 months after delivery.
There are a few risk factors that make it more likely you’ll develop varicose veins:
- Sex — Women are more likely to develop varicose veins due to hormonal changes during pregnancy, premenstruation, or menopause.
- Family history — There is a genetic factor to the development of varicose veins.
- Obesity — The added weight of obesity places more pressure on the veins in the legs and feet.
- Occupations — Jobs that require prolonged standing or sitting inhibit blood flow in the legs and feet, enabling varicose vein development.
Can Varicose Veins Be Dangerous?
Most varicose veins are simply a cosmetic nuisance. They can often be improved with exercise, elevation of the legs, or wearing compression stockings. But sometimes complications can arise from varicose veins. They are rare but require medical attention.
- Ulcers - Skin near varicose veins can form painful ulcers due to the long-term fluid buildup. This usually occurs near the ankles. A sign an ulcer is developing is a discolored spot on the skin.
- Blood clots - If there are signs of swelling in the legs, there could be a blood clot in a deep vein in the leg. This requires immediate medical attention.
- Bleeding - Varicose veins near the skin surface may burst. If this happens, medical attention is required
Are There Any Risks Involved with Varicose Vein Treatments?
The various varicose vein treatments we use at Metropolitan Vascular Institute are low risk. This is especially true when comparing it to the former common treatment method of surgical vein stripping.
Complications are very rare with endovenous laser ablation. There is a possibility of deep vein thrombosis/clotting. Nerve damage to surface sensory veins is possible, but these nerves usually return to normal in a few weeks to months.
Sclerotherapy is virtually risk free. There is a slight chance a patient can have a reaction to the sclerosant solution, but these are very, very rare.
These are safe, very effective treatments at MVI for addressing your varicose veins.
Are There Natural Treatments for Varicose Veins?
There are plenty of things you can do at home to help with existing varicose veins or to help keep new ones from forming. Here are some ideas.
- Exercise - The best option for both treating, aftercare, and prevention is exercise. Exercise boosts circulation in the legs, and this helps push along the blood that is collecting in your veins. Exercise also helps to lower your blood pressure, which is another contributing factor to varicose veins. Low impact exercise, such as walking, swimming, cycling, and yoga are all great.
- Wear compression stockings - This hosiery give your support tissues and veins some help. The compression aids the muscles and veins as they try to move the blood back up the legs to the heart.
- Diet - Salty or sodium-rich foods can cause the body to retain water, so cutting down on salty food helps to minimize water retention. Foods high in potassium can also help in this area. These foods include almonds and pistachio nuts, lentils and white beans, potatoes, leafy vegetables, and some fish.
- Eat more flavonoids - Flavonoids improve blood circulation, which will keep the blood flowing, making it less likely to pool in the veins. Flavonoids also reduce blood pressure in the arteries and can relax blood vessels. Foods that contain flavonoids include broccoli, spinach, bell peppers, and onions; citrus fruits and grapes, cherries, apples, and blueberries; cocoa; and garlic.
- Loosen up the clothing - Wearing tight-fitting clothes can restrict blood flow. Wearing flat shoes instead of heels can also be beneficial.
- Keep the legs up - When you can, elevate your legs to the same height as your heart or above. This reduces the pressure in the leg veins and gravity helps the blood to flow smoothly back to the heart.
- Massage - Use massage oils or moisturizers and gently massage the affected areas. This helps keep the blood moving through the veins.
- Keep moving - If you have to sit at work, get up regularly and move around. When you sit back down, change positions regularly. Avoid sitting with crossed legs, as this can further restrict blood flow to the legs and feet.
What Happens after My Treatment?
When your treatment is over, we’ll put you in a pair of compression stockings. These hose help ensure the vein stays closed and jumpstarts the process of the body eventually absorbing the now-unused vein. You’ll wear your stockings overnight for the first night. After that, you’ll wear them during the day for at least two weeks.
Before you leave our Waldorf offices, you’ll be directed to take a 20-30-minute walk. Then you can drive home. From there, walking at least 30 minutes each day is mandatory.
You can return to normal activities immediately but should avoid standing still for long periods, and you’ll need to avoid long-haul flights for at least 3-4 weeks.
We will have you return for an ultrasound check of your treated veins two weeks after your treatment.
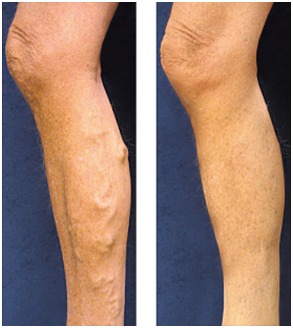
View Before and After photos of Vein Treatment
Can You Massage Varicose Veins?
As discussed in the natural treatments section, you can massage the areas with varicose veins. Don’t push directly onto the veins, however, as this can damage the blood vessels. Work all the areas around the veins.
How many Varicose Vein Treatments will I need?
Every patient who seeks varicose vein treatment may need a certain number of sessions. Treatment recommendations can vary based on the size and severity of varicose veins. Normally, we see significant improvement with 2 to 4 sessions. Appointments may be scheduled 2 to 4 weeks apart to give the body sufficient time to respond to each treatment.
After varicose vein treatment, patients may begin to see treated veins lightening within a week. However, the process can take several weeks to complete depending on the buildup of blood in the treated vein or veins.
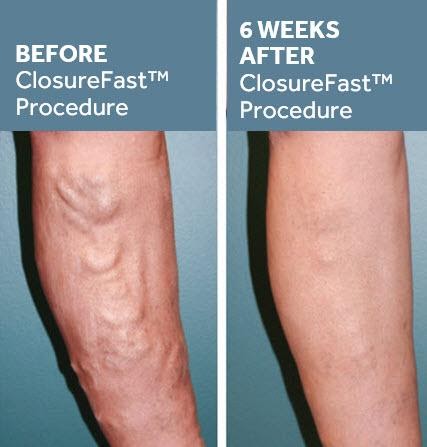
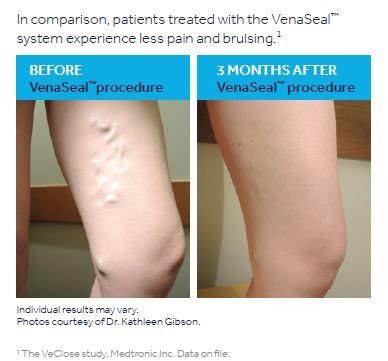
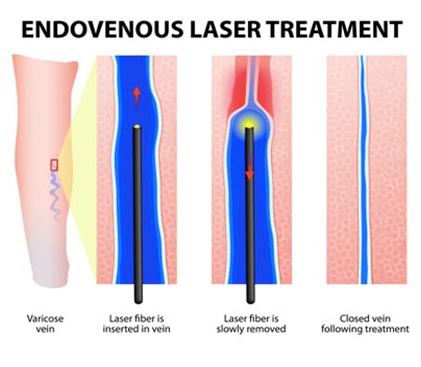
Endovenous Laser Therapy
Endovenous Laser Therapy (EVLT) or Venous Ablation is a technique that uses a laser fiber to close down the enlarged varicose veins. The procedure is performed in our office and takes about 30-45 minutes. A small laser catheter is passed into the affected vein with guidance from the ultrasound machine. The laser is then turned on and the entire vein closed down. The laser is fired at multiple locations and the entire procedure is performed with some local anesthesia.
The closed vein is reabsorbed into the body and the blood supply in that area is naturally rerouted to other veins. Recovery is rapid and involves minimal pain.
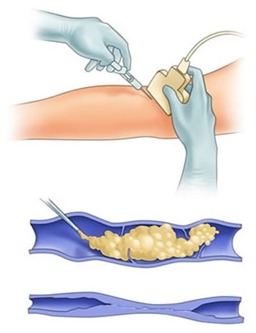
Sclerotherapy
Sclerotherapy is a minimally invasive procedure that eliminates the patient’s spider veins. Spider veins are tangled groups of tiny blood vessels just under the skin’s surface that resemble spider webs or tree branches.
Typically, they are red, blue or purple and are clearly visible on the thighs, lower legs and face.
Compression Stockings
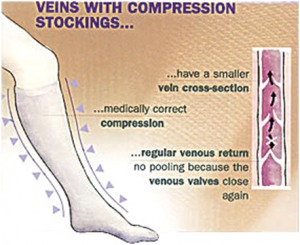
Not all situations need to be treated with an endovascular procedure. Sometimes patients can be fitted for compression stockings and followed up with subsequent ultrasound examinations.
Patients can be fitted for and purchase compression stockings in our office.
Varicose Vein during Pregnancy
Effect of Pregnancy on the Venous System
During pregnancy, many hormonal changes occur in the body that has a profound effect on the veins. Blood volume increases between 40% to 50%, while increased amounts of progesterone cause the vein walls to dilate and become less elastic.
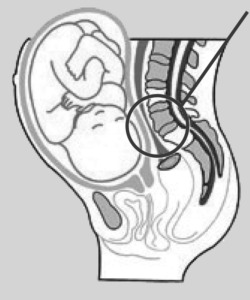
The pressure of the fetal head in the pelvis can compress the iliac veins and obstruct venous outflow from the legs. As the baby grows, the uterus enlarges and applies pressure on important veins that return blood to the heart.
This pressure can cause a slowing of the blood flow and valve damage, resulting in swelling, leg discomfort, and even varicose veins. A pregnant woman’s feet and legs may start to swell after sitting or standing for only a short time. In principle, this is a completely normal symptom.
However, if your feet are already swollen when you get up in the morning, consult your doctor. While these symptoms may subside after delivery, with each subsequent pregnancy, they are less likely to completely disappear.
Pregnant patients are encouraged to have an evaluation during pregnancy and treatment is encouraged after delivery.
Pregnancy and DVT
Women who are pregnant are at a high risk for the development of a Deep Vein Thrombosis, known as DVT. One reason is due to the increased blood volume at full term.
Additionally, pregnancy causes hormonal changes that increase blood coagulability, a measure of how easily blood clots. The expanding uterus puts pressure on blood vessels, restricting blood flow from the legs and pelvis back to the heart.
Slower blood flow increases the risk of Deep Vein Thrombosis. The risk continues during the postpartum period until the woman’s hormonal levels return to their pre-pregnancy state.
Common Leg Health Problems During Pregnancy
Venous disorders and leg health problems are among the most frequent medical conditions in North America. You may experience these conditions for the first time during pregnancy. For example, swollen feet, tired aching legs and a feeling of heaviness in the legs are among everyday symptoms that pregnant women may experience.
These symptoms are especially frequent when:
- a history of varicose veins and venous disease exists in the family
- a venous condition was already present before the pregnancy
- The woman sits and stands for prolonged periods of time while pregnant
- The woman does not exercise regularly during the pregnancy, or
- The woman has had more than one pregnancy
Pregnancy plays a role in the development of varicose veins. 30% of women pregnant for the first time, and 55% of women who have had two or more full-term pregnancies develop varicose veins.
Vascular Imaging
Ultrasound is a non-invasive imaging scan that uses sound waves to “see” inside your body. At the Metropolitan Vascular Institute, we have an expert team of physicians, nurses, and technologists who are highly trained in ultrasound imaging.
Venous Duplex Ultrasound Scan
The purpose of a venous duplex ultrasound scan is to evaluate venous blood flow in the patient’s arms and/or legs. Patients may experience symptoms such as pain, swelling or varicose veins in the arms or legs. These scans can aid in the diagnosis of venous abnormalities such as a suspected blood clot in a deep vein of the leg (DVT); narrowing or closure (occlusion) of a vein; or impaired blood flow (venous insufficiency).
Venous Doppler
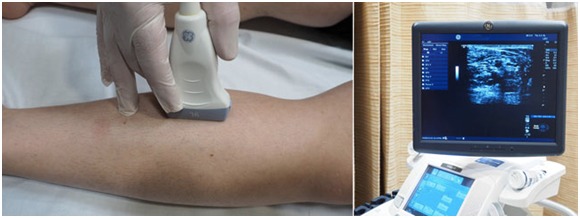
A Venous Doppler ultrasound study may be part of a venous duplex ultrasound examination. Doppler ultrasound is a special ultrasound technique that allows the physician to see and evaluate blood flow through arteries and veins in the abdomen, arms, legs, neck, or within various body organs such as the liver or kidneys.
Are there permanent treatments for Varicose Veins?
Varicose vein treatments are permanent. They also are not. Procedures like sclerotherapy and endovenous laser therapy close existing varicose veins. Once a vein is closed, it does not reopen; the vein is gradually absorbed and it disappears. That said, varicose vein treatment cannot stop new veins from forming.
After having sclerotherapy or another procedure, patients can benefit from implementing the lifestyle habits mentioned here to decrease the risk of future varicose veins. Despite these habits, venous insufficiency may once again result in ropy, bulging veins. In this instance, additional vein treatments can be performed as needed.
Will Varicose Veins go away on their own?
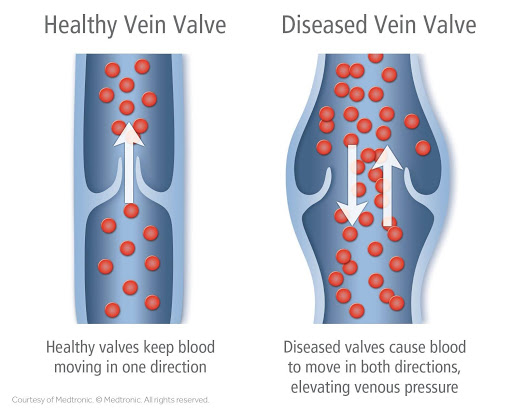
No. The only way to get rid of existing varicose veins is through medical intervention like sclerotherapy, endovenous laser treatment, or ambulatory phlebectomy.
However, there is one exception to the norm, pregnancy.
Women who develop varicose veins while pregnant may see the condition resolve in the first few months after childbirth. In this case, varicose veins are related to the way that hormones cause blood vessels to dilate, increasing blood flow. Usually, pregnancy-related varicose veins resolve within about 12 weeks after delivery.
Can Varicose Veins Be Prevented?
In short, no. Varicose veins are the product of venous insufficiency, which is the result of several contributing factors. That said, there are steps you can take to inhibit the formation of dysfunctional, painful veins. These steps include:
- Exercise several days a week. Vascular health and circulation improve with daily walks as much as they improve with more strenuous cardio exercise. Whether you ride a bike, hike, or walk, do it at least 5 days a week.
- Maintain a healthy weight. When weight increases disproportionately to our height and body frame, the vascular system is put under extraordinary stress. Regular exercise is one path to shedding extra pounds.
- Move frequently. Many people today live a relatively sedentary lifestyle. We work at desks for 9 or more hours a day. If you’re one of those people who does, set a timer to get up and walk around for 5 minutes every 60 to 90 minutes. Likewise, people who stand for prolonged periods need to schedule breaks during which they can sit or, even better, elevate their legs.
- Elevate the legs. Varicose veins develop because blood is not pushed upward toward the heart with the efficiency that is required. Elevating the legs to any degree can help blood move out of swollen, uncomfortable veins.
- Wear compression. People often mistake compression as something that one should do after vein treatment. Compression may be worn before you seek treatment and also afterward to help prevent new varicose veins from developing. It isn’t necessary to wear compression stockings all day every day. A doctor can help you determine the best time to rely on compression based on your lifestyle.
Patient Testimonial
"My experience with MVI has been a wonderful experience I have the pleasure of being the patient of Dr. Wu and Dr Gupta and their staff. They have been nothing short of a miracle. Their attentiveness and care for the patient is felt when you first meet them and I love it and the choice I made. Thank you and keep up the great work."
Schedule a Varicose Vein Consultation
Metropolitan Vascular Institute is proud to provide professional vein treatment care in a friendly environment. Call our Waldorf, MD office at (301) 374-8540 to schedule your visit, or click here to send us an appointment request form. Our experienced providers look forward to serving you!