
From surgical creation of dialysis access to minimally invasive procedures to help maintain a healthy access, our expert staff aim to navigate you through your journey as we work closely with your nephrologists/dialysis centers.
Vein Mapping
Mapping of arm vessels before the surgical creation of dialysis access has been shown to help achieve higher arteriovenous fistula (AVF) rates as well as an improved fistula success rate.
This is performed in the office using ultrasound and is painless. Our board-registered Vascular Technologist, with years of experience, will perform the examination. The exam takes 45-60 minutes.
Tunneled Catheter (Perma-catheter) Placement, Exchange & Removal
A hemodialysis catheter is a hollow tube used for removal and replacing blood to and from your body. The catheter is tunneled from the internal jugular (IJ) with the tip entering the atrium of the heart. An exit site for the catheter is in the chest wall, under the collar bone. A small cuff on the catheter at the exit site sits under the skin. This cuff helps to keep the catheter in place, as well as, help prevent bacteria from entering the body.
The end of the catheter (outside of the exit site) known as a hub has 2 lumen. One lumen carries blood to the dialysis machine, while the other brings blood back into the body once it has been cleansed by the machine. Each lumen has a clip and an end cap that prevent air from getting into or blood from leaking out of the catheter. We can perform hemodialysis catheter placements, exchanges and removals in our office.
Fistulagram
This is a minimally invasive procedure in which a small tube known as a sheath is inserted into the fistula. Through this sheath, we are able to administer sedative medication and perform diagnostic and therapeutic interventions. X-rays are taken to identify narrow areas (stenoses) within your fistula/graft. If stenoses are identified a balloon can be used to widen the narrowing (angioplasty) to restore improved flow in your fistula/graft.
Thrombectomy
If your fistula/graft clots, a procedure similar to a Fistulagram is performed to remove all the clot and restore the adequate flow in your fistula/graft.
Stenting
There are times when angioplasty (ballooning) is ineffective and a stent may be placed. A stent is a spring metal mesh placed inside the vein or graft to keep the vein/graft open.
Fistula Maturation
Once a fistula is created (vein is connected to the side of an artery), it usually takes about 2 months before the fistula is mature and ready to start using for dialysis. If the fistula is slow to mature, a fistulagram is done to identify the cause. If there is a narrow area present limiting flow in the fistula, balloon angioplasty will be performed to promote maturation. Sometimes there are large branches present taking flow away from the fistula. If this is causing the fistula to be slow to mature, a coil can be placed into this branch to stop flow in the branch in order to have all the flow going into the fistula.
What are the different types of dialysis treatments for kidney disease?
There are two types of dialysis, hemodialysis and peritoneal disease.
- Hemodialysis — With hemodialysis, a machine removes blood from your body, filters it through a dialyzer (an artificial kidney), and returns the cleaned blood to your body. This is a 3- to 5-hour process and is performed at a hospital or a dialysis center three times a week.
Hemodialysis can also be done at home. These treatments require more frequency, typically between four and seven times a week, but they don’t take as much time. Some patients opt to do their home hemodialysis at night while they sleep.
- Peritoneal dialysis— With peritoneal dialysis, tiny blood vessels inside your abdomen lining (peritoneum) filter blood through the aid of a dialysis solution. This solution is a type of cleansing liquid that contains water, salt, and other additives.
Peritoneal dialysis is done at home using either of these methods:
- Automated peritoneal dialysis uses a machine called a cycler.
- Continuous ambulatory peritoneal dialysis is done manually.
How accessible are dialysis clinics?
There are over 7,500 dialysis clinics in the United States. The prevalence of chronic kidney disease has been increasing in the United States since the 1960s. As the incidence of chronic kidney disease has increased, so has the number of dialysis centers to serve these patients.

The primary causes of chronic kidney disease include diabetes, high blood pressure, polycystic kidney disease, long-term autoimmune attack, and prolonged urinary tract obstruction. The final stage of kidney disease is known as end stage renal disease (ESRD). When a patient reaches this stage, he or she must either receive a kidney transplant or undergo regular dialysis treatment.
What are the Warning Signs?
A Functioning Vascular Access is Vital for Dialysis. Warning Signs Your Access May Be Failing –
Fistula/Graft
- Prolonged Bleeding
- Pain
- Difficult Cannulation
- Arm Swelling
- Aneurysm Formation/Growth
- High Venous Pressures
- No Thrill/Change in Thrill
- Infiltration
- Non-maturing Fistula
- Redness/Drainage
- Poor Clearance
- Clotting of Needles or Lines
- Abnormal Arterial Pressures
- Recirculation
- Poor Flow
Catheter:
- Pain
- Poor Catheter Flow (less than 300ml/min)
- Redness/Drainage
- Poor Clearance
- Clotting of Lines
- Recirculation
- Unable to Aspirate
If you notice ANY of these symptoms, please inform your doctor or nurse immediately.
What if I own a Catheter?
- Keep site clean and dry
- Dressing changes will be done at dialysis center
- Transition to a fistula or a graft as soon as possible
How long will I need to receive dialysis?
If you had a sudden kidney injury and shutdown, you may only need dialysis for a short time until your kidneys recover. But if you have chronic kidney disease the kidneys rarely improve. In these cases, you’ll either need to be on dialysis permanently or you’ll need a kidney transplant.
How often do I need to receive dialysis?
Usually, dialysis needs to be done three times per week with each session taking from 3 to 5 hours. These are conventional hemodialysis treatments at a hospital or dialysis clinic. Daily hemodialysis doesn’t take as long, but it requires more frequent treatment sessions, about six per week.
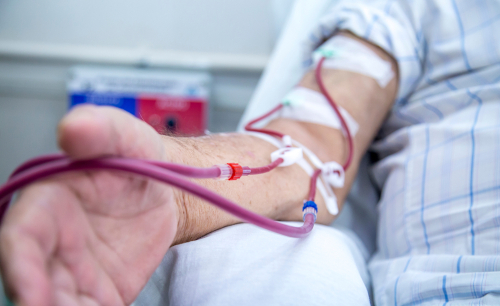
Is a dialysis session painful?
Dialysis treatments are painless. Some patients may have a drop in their blood pressure that could lead to nausea, vomiting, headaches, or cramps, but these are not typical.
Are there any alternatives to dialysis?
Dialysis is time-consuming and expensive. There are other options that may help to manage your symptoms. One of these is anemia management. When your kidneys are working properly, the hormone erythropoietin (EPO) is produced naturally in the body. To help with an under-functioning kidney, you can receive an EPO injection every week.
Keeping your blood pressure in a healthy range can slow the deterioration of your kidneys. Drink fluids to avoid dehydration. Be careful about your use of anti-inflammatory medications.
A kidney transplant is another alternative. Some people do not qualify for a kidney transplant, however, if they…
- Smoke
- Are heavy alcohol users
- Are obese
- Have an untreated mental condition
What can I do to keep my dialysis access healthy?
- Examine your access daily to ensure there is a thrill
- Keep site clean
- Wash skin daily with soap and water
- Avoid sleeping on your access arm
- Avoid carrying heavy objects with your access arm
- Avoid checking blood pressure on your access arm
Patient Testimonials:
"Staff was wonderful! They took excellent care to make sure I was comfortable. They explained the procedure. Dr. Nwosu has excellent bed side manor and cares. He knew I was nervous and helped to reassure I was in good hands and everything would be fine. I would recommend this center and would return"
Schedule a Client Consultation
If you are interested in learning more about Dialysis access and ESRD services, please call our office at (301) 374-8540 or fill out a form below to get started!

